UT Health East Texas Neurological Institute
UT Health East Texas Neurological Institute offers access to high-level treatment of the brain, spine and neurological system. Neurological specialists are available 24/7 and provide a wide range of specialties, allowing patients to receive the care they need at a comfortable and convenient location.
Medical treatments and technologies used at the center include CyberKnife Radiosurgery, sterotactic neuronavigation, The Penumbra system, Medtronic StealthStation, brain endoscopy, brain mapping and awake brain surgery. These advanced procedures and tools allow for better treatment outcomes and faster recovery for the patient.
Our Specialists
Our team of board-certified neurologists, neurosurgeons and specialized technicians are committed to patient-focused care. Their expertise covers a wide range of specialties:
- Conservative spine treatment
- Epilepsy treatment
- Movement disorders (including Parkinson’s)
- Neurological Oncology
- Stroke Care
- Neurological surgery and trauma
- Neuroradiology and Interventional Neuroradiology
- Pain Management
- Rehabilitation
Our flagship stroke program at UT Health Tyler is certified by the Joint Commission as a primary stroke center. The first hospital in East Texas to have a certified stroke center, the program has gone on to receive recognition and awards for their effort to ensure high quality care.
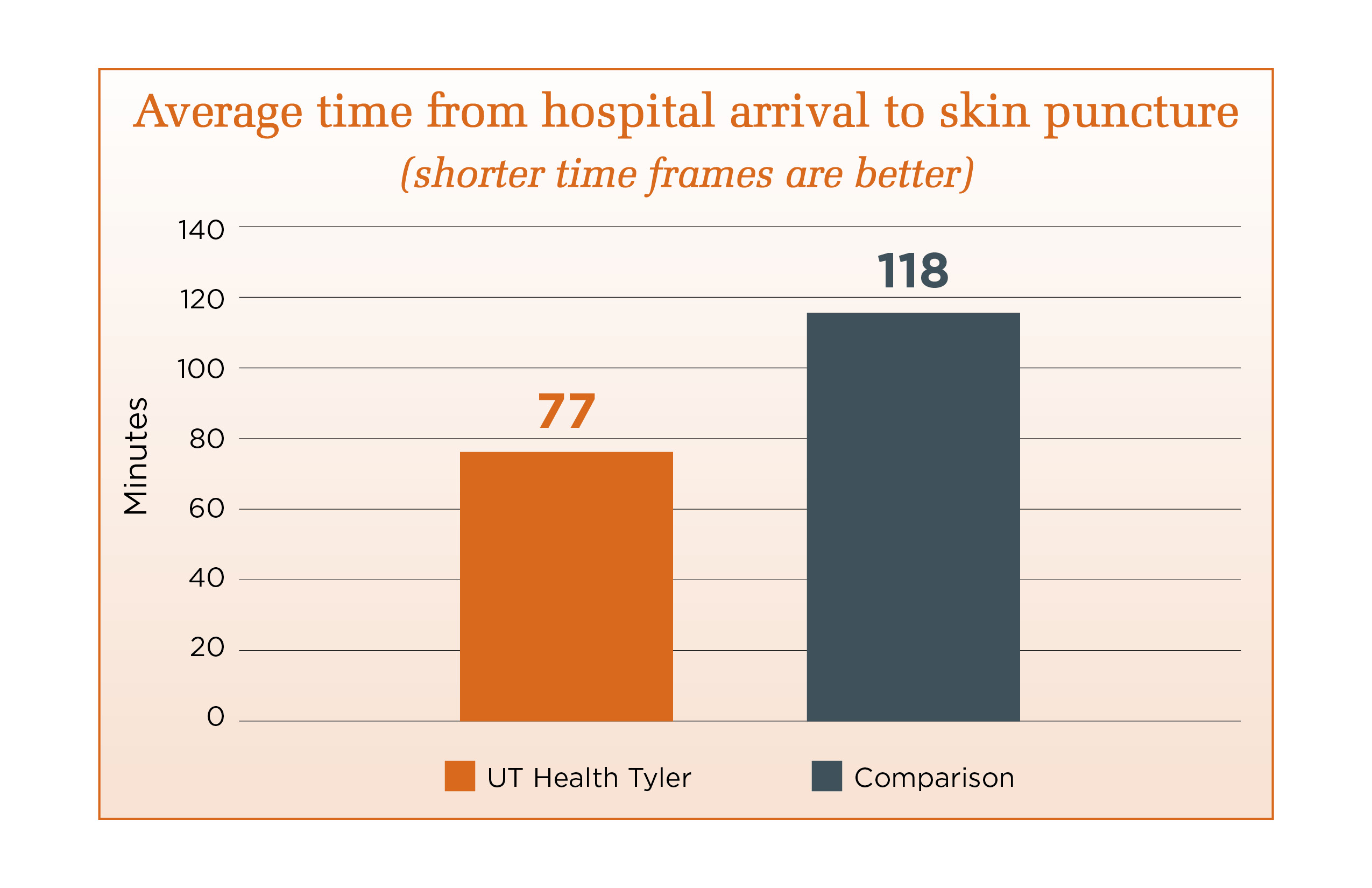
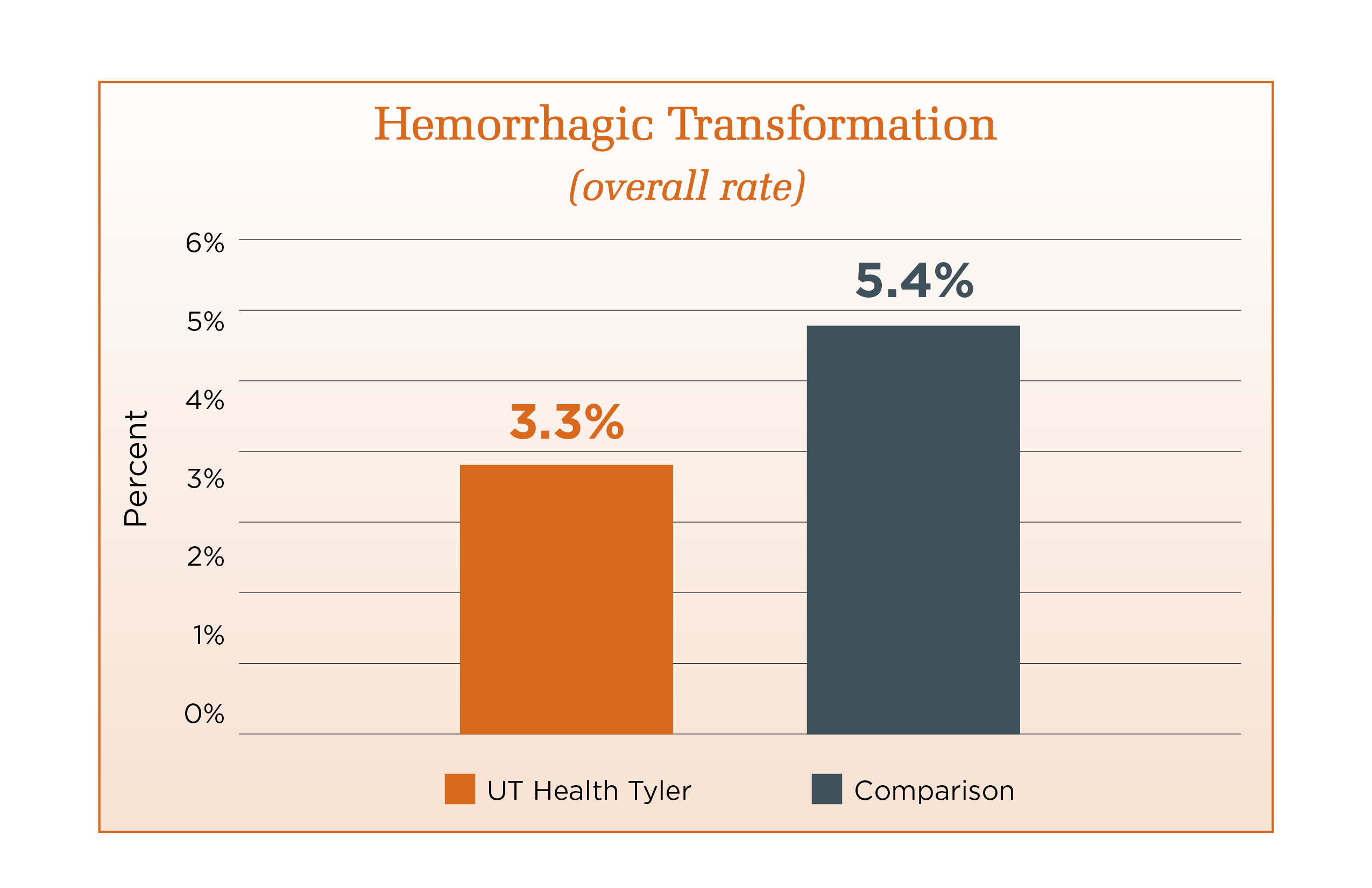
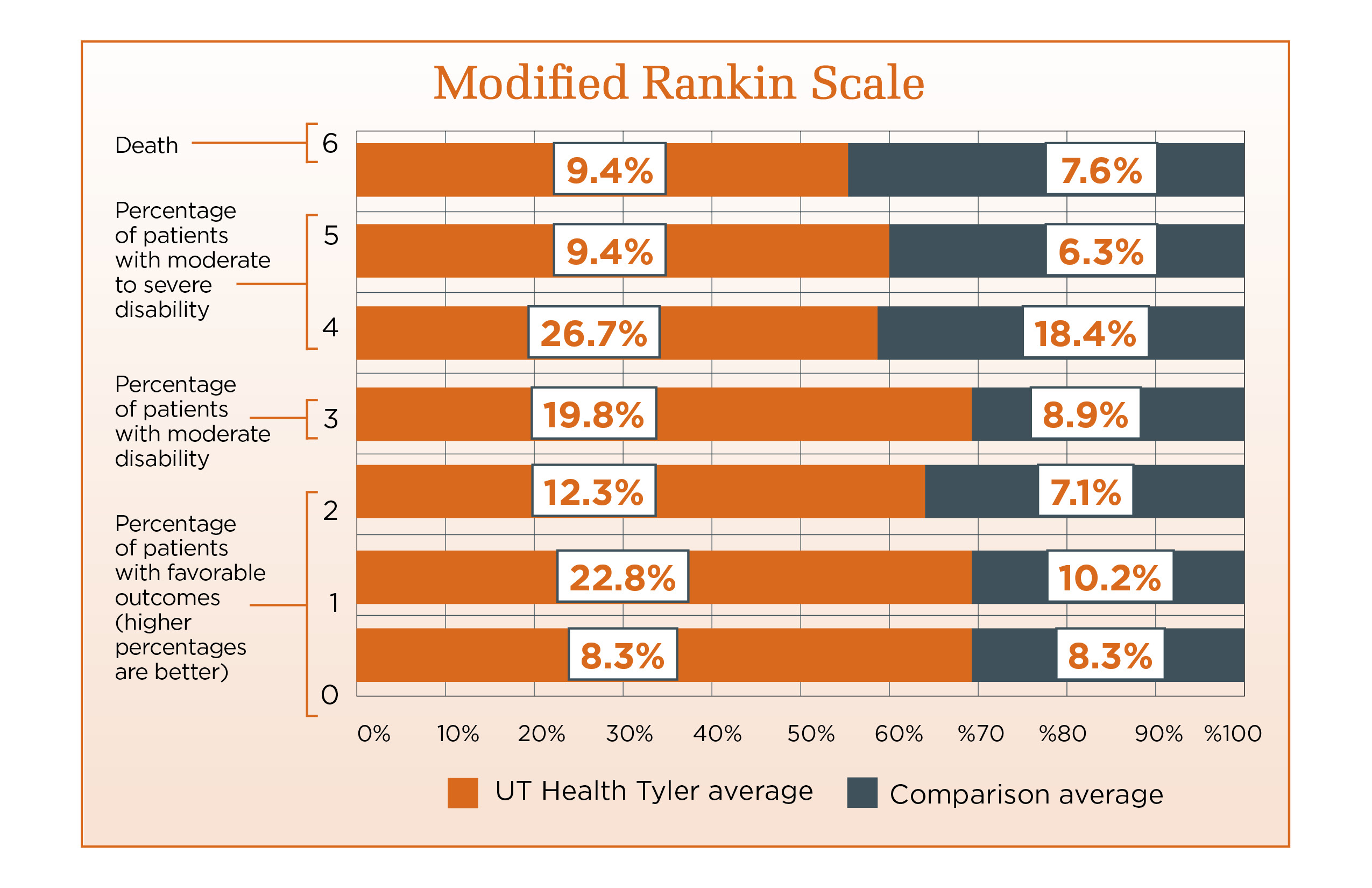
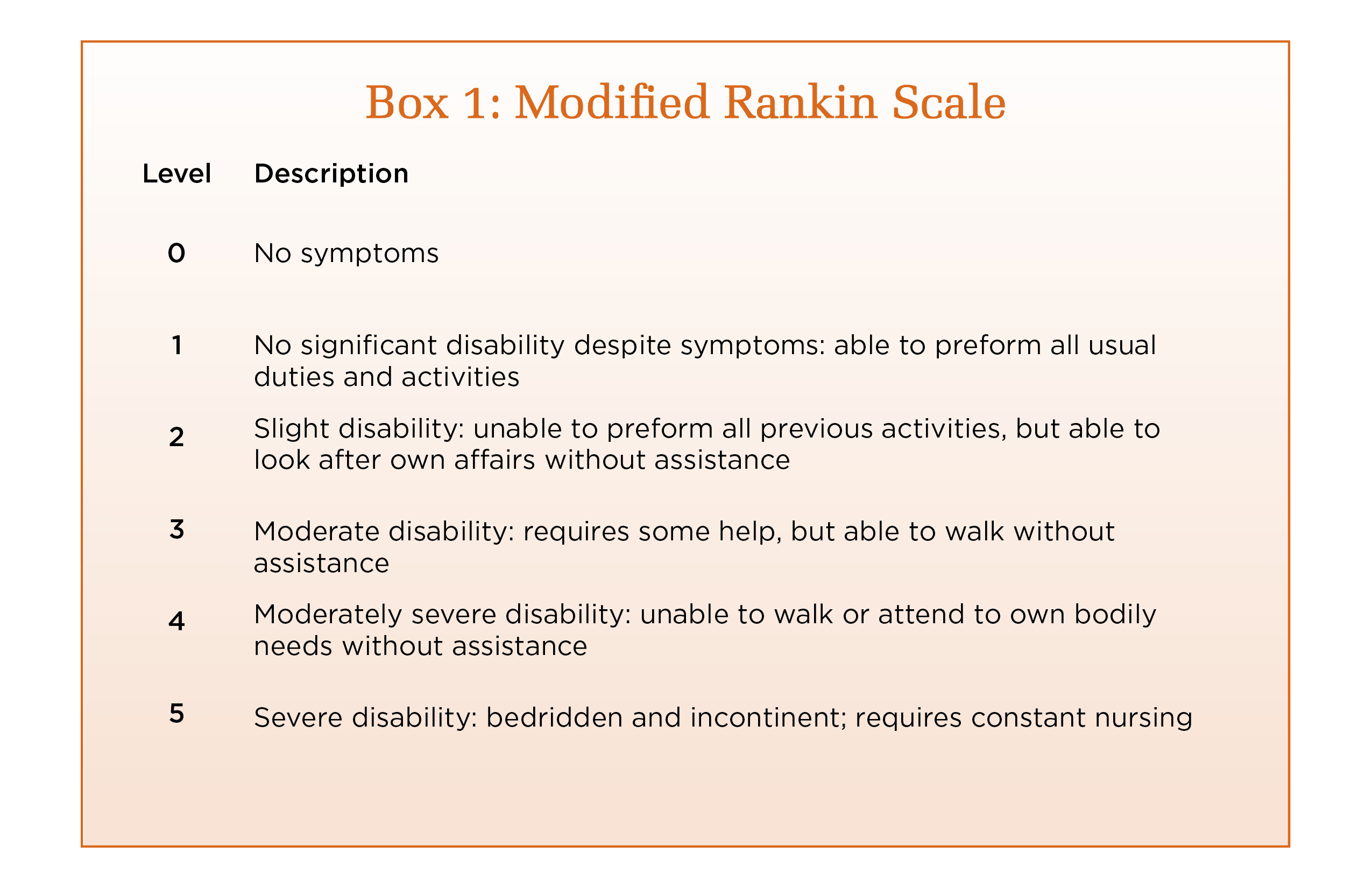
Stroke Performance Measures
-
Joint Commission-certified Comprehensive Stroke Center
UT Health Tyler has earned The Joint Commission's Gold Seal of Approval® and the American Stroke Association's Heart-Check mark for Comprehensive Stroke Certification. This certification recognizes the significant commitment of resources comprehensive stroke centers must have to treat complex stroke. UT Health Tyler prepared for the certification process by offering its patients the latest approaches for caring for brain aneurysms, including coilings, clippings and flow diversions. UT Health Tyler has the ability to care for the most acute and complex patients. This is possible with state-of-the-art neurointerventional angiography and advanced imaging tools. Our specialized stroke team manages the stroke patient from the onset of the stroke to rehabilitation and then management post stroke.
For our full 2024 Patient Stroke Outcomes Report, click here.
Mortality Rates:
Another important outcome measure is the mortality rate associated with key interventional procedures to help people who suffer strokes or to prevent a future stroke.
A Carotid Endarterectomy is a procedure to treat poor blood flow in a patient’s carotid artery. The Carotid Endarterectomy mortality rate at discharge is 0% since January 2019 and the 30 Day Carotid Endarterectomy rate is also 0% since January 2019.
We make care for our patients a priority. That’s why we provide our patients with a variety of services to support them during their stay and treatment. Support services include case managers, chaplains, nutritionists, pharmacists, Home Health services, psychiatrists, social works and support groups. To view 2019 neurological support groups location and dates, please visit our Facebook page.
For more information about treatments available or for a physician referral, please call the UT Health East Texas Neurological Institute at 903-535-6092.